Frequently Asked Questions
Medical aid in dying laws are in effect in Oregon, Washington, California, Colorado, New Mexico, New Jersey, Vermont, Maine, Hawaii, Delaware, and the District of Columbia (Montana also has it by court decision). That means this basic human right is already extended to some 73 million Americans. Arizona is lagging behind.
The term “physician-assisted suicide” has been used in the past as if it were a synonym for medical aid in dying, but the terms are not at all equivalent. “Physician-assisted suicide” is used in a negative and biased way by opposition groups in an attempt to stigmatize the issue, and is sometimes still used in media reports because reporters may not be aware that the term is not accurate.
These laws specifically state that medical aid in dying is not suicide or assisted suicide. A death with medical aid, for example, is covered by insurance policies that have clauses disallowing coverage for suicide. The death certificate also will not list suicide as the cause of death, but will list the terminal illness as the cause.
It really isn’t suicide if you are dying anyway. Persons using the medical aid in dying option generally would want to extend their lives if it were possible—they just don’t want to extend their deaths. They simply want some control over the inevitable dying process.
Terminally ill patients who legally access medical aid in dying in other states also find the word “suicide” offensive and hurtful. Many have publicly expressed that the term is hurtful and derogatory to them and their loved ones.
In addition, professional organizations like the American Psychological Association, the American Public Health Association, and the American Association of Suicidology draw sharp distinctions between medical aid in dying and suicide. Suicides are often violent, traumatic, and shocking. Medical aid in dying is specifically intended to be peaceful and humane. There is a world of difference.
The American Association of Suicidology has stated: “In general, suicide and physician aid in dying are conceptually, medically, and legally different phenomena…. The American Association of Suicidology is dedicated to preventing suicide, but this has no bearing on the reflective, anticipated death a physician may legally help a dying patient facilitate…. In fact, we believe that the term ‘physician-assisted suicide’ in itself constitutes a critical reason why these distinct death categories are so often conflated, and should be deleted from use. Such deaths should not be considered to be cases of suicide and are therefore a matter outside the central focus of the AAS.”
Right now, nobody in Arizona is eligible for medical aid in dying! Should the proposed law be enacted, it would be available to any adult resident of the state deemed to be terminally ill (six months or less to live), who is able to make informed decisions, and who is capable of ingesting the prescribed medication on their own.
Data and studies show that the safeguards in these laws work as intended, protecting patients and preventing misuse. No evidence of coercion or abuse has been documented since the first such law took effect in 1997.
The law includes the following safeguards:
- Patients must meet stringent eligibility requirements, including being an adult, a state resident, mentally competent, and having a terminal diagnosis with a six-month prognosis as confirmed by two licensed physicians.
- The patient must be informed by the attending physician of the diagnosis, the prognosis, the nature of the medication to be prescribed, and other alternatives, including comfort care, hospice care and pain control.
- The patient must make two separate requests for medication, oral and written.
- Only the patient him or herself can make the oral and written requests for medication, in person. It is impossible to stipulate the request in an advance directive, living will, or any other end-of-life care document.
- The patient must wait at least 15 days before getting the medication. It cannot be a spur of the moment decision.
- The written request must be witnessed by at least two people, who, in the presence of the patient, attest that to the best of their knowledge and belief the patient is capable, acting voluntarily, and is not being coerced to sign the request. One of the witnesses cannot be a relative of the patient by blood, marriage or adoption, or anyone who would be entitled to any portion of the patient’s estate.
- The patient must be deemed capable to take (self-administer and ingest) the medication themselves, without assistance, which assures it is a voluntary act.
- The patient may rescind the request at any time.
- Two physicians, one of whom is the patient’s attending physician, must confirm the diagnosis. Each physician must be licensed by the state to practice medicine and certified to prescribe medications.
- If either physician determines the patient may be suffering from a psychiatric or psychological disorder or depression causing impaired judgment, they must refer the patient for evaluation by a state licensed psychiatrist or psychologist to determine their mental competency. Medication cannot be prescribed until such evaluation determines the patient is mentally competent.
- The physicians must meet strict reporting requirements for each request.
- Anyone who falsifies a request, destroys a rescission of a request, or who coerces or exerts undue influence on a patient to request medication under the law commits a Class 2 felony.
Yes. The American public consistently supports medical aid in dying by significant majorities in both national and state surveys across almost all demographic groups.
____________________
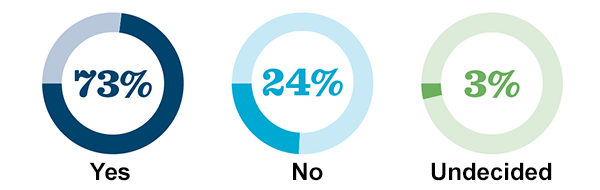
AMONG ALL ADULTS
AGREE: “When a person has a disease that cannot be cured…doctors should be allowed by law to end the patient’s life by some painless means if the patient and his or her family request it.” (Gallup Poll, June 2017)
____________________
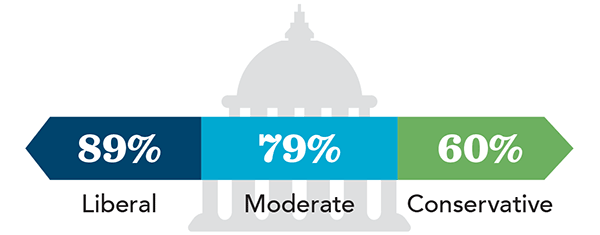
AMONG POLITICAL IDEOLOGIES
AGREE: “When a person has a disease that cannot be cured…doctors should be allowed by law to end the patient’s life by some painless means if the patient and his or her family request it.” (Gallup Poll, May 2017)
____________________
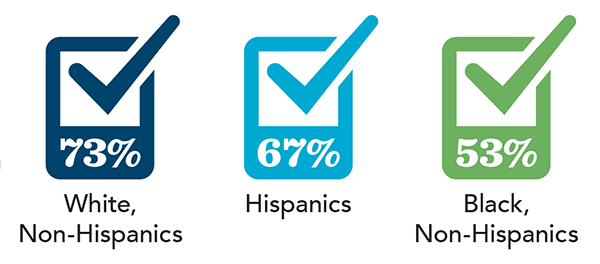
AMONG ETHNIC GROUPS
AGREE: “When a person is facing a terminal disease, it is morally acceptable to ask for a physician’s aid in taking his or her own life.” (LifeWay Research, September-October 2016)
____________________
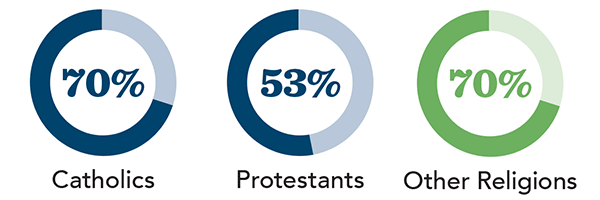
AMONG RELIGIOUS AFFILIATIONS
AGREE: “When a person is facing a terminal disease, it is morally acceptable to ask for a physician’s aid in taking his or her own life.” (LifeWay Research, September-October 2016)
____________________
AMONG AGE GROUPS
AGREE: “Individuals who are terminally ill, in great pain and who have no chance for recovery have the right to choose to end their own life.” (Gallup Poll, May 2015)
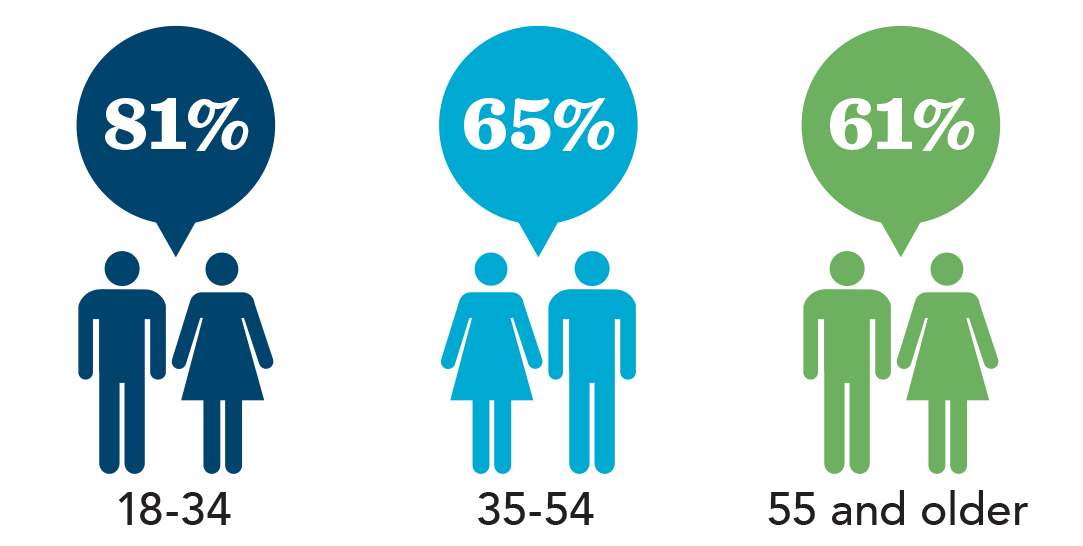
There are many people who have sincere and deeply held beliefs against medical aid in dying. These beliefs should be fully respected and honored. We have absolutely no quarrel with these beliefs.
The only problem is that there is a significant minority of such people who insist on forcing their beliefs on everyone else. And this minority is very motivated, very politically active, very well organized, and very well funded—all characteristics that the “silent majority” seems to lack.
Supporters of medical aid in dying have the opposite mentality. Such people are 100% supportive of those who do not want to participate in medical aid in dying. Medical aid in dying is totally voluntary. No patient need participate. No doctor need participate. No health care facility need participate. There is no forcing of belief or action on anyone.
We have the moral high ground on this issue. It is human freedom that is at stake here.
It is worth repeating the words of the Federal Ninth Circuit (which includes Arizona) in Compassion in Dying v. Washington, 1996:
“Those who believe strongly that death must come without physician assistance should be free to follow that creed, whether they be doctors or patients. But they should not be free to force their views, their religious convictions, or their philosophies on all other members of a democratic society, nor should they be free to compel those whose values differ from theirs to die painful, protracted, and agonizing deaths.” — Ninth Circuit Court of Appeals
Finding your legislators
We have new legislative districts in 2022, so if you do not know your new state legislative district number, you can find it by entering your address in the box at the upper left at the AZ Official Legislative Map website.
Once you have your state district number, you can go to the Arizona State Legislature Member Roster to find the name and contact information for your two State Representatives and your one State Senator. You can click on District Number to sort by district, and click on Senate Roster to get your Senator.
Communicating with legislators
The following advice is from a former state legislator who is a strong supporter of our cause. Unfortunately, in-person meetings with legislators are on indefinite hold due to the coronavirus pandemic.
Email is the least effective method of communication because legislators are inundated with it and will simply ignore most of it (you would too!). If you do use email, send to your own legislator and indicate in the subject line what district you live in. Be brief and to the point. If you send an email to several or even all 90 legislators, be sure to mail them separately or use the BCC (blind carbon copy) field so it appears that you are emailing only one legislator. If there are 90 legislators in the “To” field, your message will surely be ignored.
Telephone is the second least effective means. Again, the reason is that legislators are just too busy. If you do call, leave a message with your name and address (so they know you are in their district), and a very brief message (for example, that you would like them to vote for or against your item of interest). You may also use the telephone, of course, to request a face-to-face meeting (see below).
A letter or fax is the next most effective way to communicate with legislators. There is no difference in effectiveness between a letter or fax, so if time is short use a fax. Always say “I am a registered voter in your district” or the equivalent. Never use a form letter or photocopy. Handwritten letters are just as good if not better than typewritten ones. As in any communication, it is best to be brief and very much to the point. Keep your letter to one page at the very most. The very best letters are personalized — how YOU are affected by whatever issue you are writing about.
Face to face communication is the most effective [but unfortunately is not currently practical due to the Covid 19 pandemic]. You can request a personal meeting with your own legislators to express your concerns, and you may call to make an appointment. You can also do this in small groups. If getting to Phoenix is difficult you can request a meeting when your legislator is back in your district (most are home on Fridays or weekends, but members of the Appropriations Committee also work in Phoenix on Fridays). There is also an office in Tucson (400 West Congress) where meetings can be arranged with legislators from Southern Arizona. When meeting a legislator, especially in Phoenix, you should be very patient. They are very busy (like doctors) and often overbook their appointments. They can also be called away suddenly to unscheduled business on the floor. Mondays are usually the least hectic days for legislators.
Even more effective than requesting a face to face meeting is to develop a relationship with your legislator, if possible, so you know something about them as a person and they also know you as a person. If you have this type of relationship, they are much more willing to give you an audience and consideration for things you might have to say. This is basic human relationship building.










